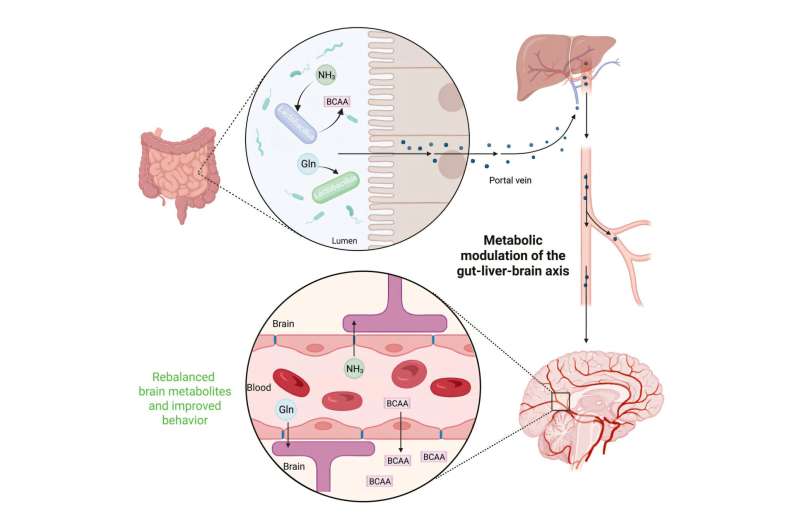
When the liver fails, toxins—such as ammonia—that should be filtered from the blood build up and reach the brain. The result is hepatic encephalopathy (HE), a devastating neurological complication of liver disease that can cause anxiety, confusion, memory loss and, in severe cases, coma. HE is a common endpoint of liver cirrhosis, driving frequent hospitalizations and placing a heavy burden on patients and health care systems worldwide.
Current treatments offer only partial relief. The two mainstay therapies—lactulose and the antibiotic rifaximin—work primarily by reducing ammonia production in the gut, but neither corrects the full spectrum of metabolic disruptions that drive the disease. Patients remain vulnerable to recurrence, and rifaximin carries the added risk of disrupting the gut’s natural microbiome. A fundamentally different approach is needed—one that can tackle several disease drivers at the same time.